
Continuation of Risks of Trabeculectomy (Part 1 of 2)
Late postoperative (after the eye has healed from surgery)
Loss of vision
Many patients who need to have glaucoma surgery have already lost a significant amount of vision. They would be expected to lose additional vision without glaucoma surgery. Nevertheless, in one study almost 14% of patient who had trabeculectomy with Mitomycin-C (MMC) lost vision due to complications of surgery.[1] This risk may be lower in those who have glaucoma surgery without use of MMC. Some of the causes of vision loss after trabeculectomy are as follows:
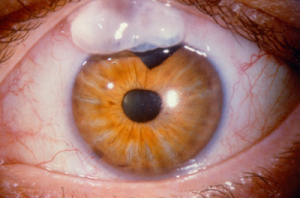 Failure of the bleb
Failure of the bleb
Although on average trabeculectomies “fail” at a rate of approximately 10% per year, some blebs continue to work even twenty years after surgery. Such long-standing blebs would likely not be possible without the modern use of antimetabolites such as Mitomycin-C (MMC) to limit scarring of the bleb.
Leaking bleb
The use of MMC works very well to prevent scarring (failure) of a bleb. However, it also results in paper-thin delicate blebs which are prone to leak and are easily damaged. When MMC is used during trabeculectomy, there is about a 15% risk of bleb leak in the first five years after surgery.[1] Bleb leaks can lead to hypotony (as well as the problems associated with hypotony) and may even progress to infection of the inside of the eye.
Hypotony Maculopathy
An IOP that is too low (hypotony) can occur at any time after trabeculectomy. When it is not successfully treated, long term hypotony can lead to central retinal (macular) damage called hyptony maculopathy. This risk increases as the risk of hyptony increases. One of the main risks of developing hypotony is the use of Mitomycin-C. In one study of patients who underwent trabeculectomy with MMC, 9% of patients developed hypotony maculopathy at some point during the five years of follow up after surgery.[1]
Infection
With most eye surgeries the risk of infection is greatest early after the surgery is performed. Once the eye has healed the risk of infection due to surgery is essentially zero. Not so with trabeculectomy. Because use of MMC results in thin, delicate blebs and severely limits the body’s healing response, any damage to the bleb could result in a small opening that would allow bacteria into the eye. Infections can range from “blebitis” to severe, vision-threatening infection of the entire eye (endophthalmitis).
Blebitis is just what it sounds like: an infection limited to the bleb itself. Approximately 6% of blebs will become infected in the first five years after trabeculectomy.[1] If caught early it can often be treated with only topical antibiotics. Vision can be saved at this stage in the infection.[2] Thus, it is critical that anyone who has had a trabeculectomy inform their surgeon at the earliest onset of redness, pain, or loss of vision in the eye that has had surgery.
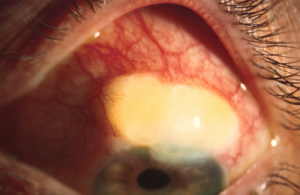 Blebitis can rapidly progress to a more serious infection of the entire eye as bacteria enter the eye through the trabeculectomy fistula. Rates of endophthalmitis have been reported to be as high as 1% per year.[3] If not successfully treated endophthalmitis often leads to severe loss of vision or blindness. This risk continues for the life of the patient unless the bleb scars down (fails).
Blebitis can rapidly progress to a more serious infection of the entire eye as bacteria enter the eye through the trabeculectomy fistula. Rates of endophthalmitis have been reported to be as high as 1% per year.[3] If not successfully treated endophthalmitis often leads to severe loss of vision or blindness. This risk continues for the life of the patient unless the bleb scars down (fails).
Cataract
It is one of the unfortunate ironies of glaucoma filtering surgery that in order to save vision one must risk losing vision. A little over forty years ago it was thought that about one third of patients who had trabeculectomy would go on to develop cataracts[4] More recent evidence suggests that number may be even higher than 50%.[1] Normally this would not be such a bad thing as most everyone eventually develops a cataract anyway and cataract surgery is one of the safest of eye surgeries. The problem is that reduced bleb function or even bleb failure is more likely after cataract surgery. So, removing the cataract to improve vision could result in IOP elevation[5] possibly requiring use of additional IOP lowering medications[6] and risking further loss of vision. It’s an unfortunate Catch-22 for patients considering trabeculectomy.
Less Severe (but nevertheless potentially bothersome) risks
Chronic Irritation
Fluid in the bleb exerts pressure on the thin bleb wall which can result in a bubble-shaped bleb. These can cause or worsen Dry Eye Syndrome resulting in chronic irritation, tearing, and blurred vision. This may be treated with artificial tears though often with limited effect.
Eyelid changes
Although most people do not notice any difference in eyelid position after glaucoma surgery, it is possible for the upper eyelid to be notably raised[7] or drooped[8] after trabeculectomy.
Risk Summary
Bleb-dependent glaucoma filtration surgeries such as trabeculectomy can be associated with numerous complications including infection, vision loss, bleb leak, bleb scarring, hypotony , cataract and the need for subsequent surgery.[9] The decision to proceed with trabeculectomy is never easy for the patient with glaucoma. For some, this may be the only surgery with a reasonable chance of controlling their glaucoma. Many, however, many find that their glaucoma can be successfully treated with a combination of drops and less risky surgical options.
References
1) Bindlish R, Condon GP, Schlosser JD, et al. Efficacy and safety of mitomycin-C in primary trabeculectomy: five-year follow-up. Ophthalmology. 2002;109(7):1336-1341; discussion 1341-1342.
2) Ayyala RS, Bellows AR, Thomas JV, et al. Bleb infections: clinically different courses of “blebitis” and endophthalmitis. Ophthalmic Surg Lasers. 1997;28(6):452-460.
3) Greenfield DS, Suñer IJ, Miller MP, Kangas TA, Palmberg PF, Flynn HW Jr. Endophthalmitis after filtering surgery with mitomycin. Arch Ophthalmol 1996;114:943-949.
4) Sugar HS. Postoperative cataract in successfully filtering glaucomatous eyes. Am J Ophthalmol. 1970;69(5):740-746.
5) Manoj B, Chako D, Khan MY. Effect of extracapsular cataract extraction and phacoemulsification performed after trabeculectomy on intraocular pressure. J Cataract Refract Surg. 2000;26:75-78.
6) Casson R, Rahman R, Salmon JF. Phacoemulsification with intraocular lens implantation after trabeculectomy. J Glaucoma. 2002;11:429-433.
7) Putterman AM, Urist MJ. Upper eyelid retraction after glaucoma filtering procedures. Ann Ophthalmol. 1975;7(2):263-266
8) Song MS, Shin DH, Spoor TC. Incidence of ptosis following trabeculectomy: a comparative study. Korean J Ophthalmol. 1996;10(2):97-103.
9) Lichter PR, Musch DC, Gillespie BW, et al. Interim Clinical Outcomes in The Collaborative Initial Glaucoma Treatment Study Comparing Initial Treatment Randomized to Medications or Surgery. Ophthalmology 2001;108:1943-53
DeBry PW, Perkins TW, Heatley G, et al. Incidence of late-onset bleb-related complications following trabeculectomy with mitomycin. Arch Ophthalmol 2002;120:297-300.
Don’t delay getting checked for glaucoma.
Make an appointment with an eye doctor in your area now. If you live in the greater Los Angeles area and would like Dr. Richardson to evaluate your eyes for glaucoma call 626-289-7856 now. No referral required. Appointments are available, Tuesday through Saturday.
In The Same Series:
- Trabeculectomy Surgery For Glaucoma
- Why Trabeculectomy is the Most Common Glaucoma Surgery
- Risks of Trabeculectomy (Part 1 of 2)
- Risks of Trabeculectomy (Part 2 of 2)
- When Should Trabeculectomy Be Considered?
Related Articles:
- What Is The Big Deal About A Bleb?
- Is Trabeculectomy an Option After Canaloplasty?
- PhacoCanaloplasty™ vs Phacotrab
- 1 in 5 Trabeculectomy Patients May End up With Ptosis (Eyelid Droop)
- Trabeculectomy versus Canaloplasty (TVC study)
- Trabeculectomy Glaucoma Surgery After Canaloplasty
- Trabeculectomy Glaucoma Surgery (Part 3 of 12 of “What’s New In Glaucoma Surgery” Presentation)


