A New Intraocular Pressure (IOP) Monitoring Device
An ideal intraocular pressure (IOP) monitoring device would be one that stayed in contact with the eye throughout the day and night. Given that contact lenses are easy to use and well tolerated by most it should come as no surprise that someone came up with the idea to use a contact lens to measure IOP. It is surprising, however, that a team of engineers have already figured out how to miniaturize the necessary components and embed them into a contact lens. Even more surprising is that this device, called the SENSIMED Triggerfish® Sensor device is already being used in Europe and has received CE certification.
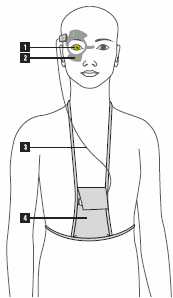
[Photo Credit: www.sensimed.ch [1] contact lens with sensor [2] adhesive antenna [3] cable [4] portable recorder]
I first mentioned the Triggerfish® here: Automated Contact Lenses To Revolutionize Glaucoma Treatment In The US Soon. At that time I was naively optimistic that this intraocular pressure device would gain FDA approval “soon.” I now know better than to believe the FDA will approve anything in a timely fashion. So, what exactly is this intraocular pressure (IOP) monitoring device for glaucoma patients that is available throughout Europe and that we hope will someday be available in the USA?
SENSIMED Triggerfish® Sensor Device For Glaucoma Patients
This SENSIMED Triggerfish® Sensor device is a silicon contact lens that has the following two miniaturized components embedded within it:
1) Strain gauge – This measures changes in the surface of the eye that correlate with IOP[1]
2) Radio frequency transmitter – This sends a signal to an antenna that is worn by the patient
Amazed? I am. However, before you rush out to your glaucoma specialist there are a few things you should know:
1) The strain gauge measures changes in the surface of the eye that correlate with IOP. However, the actual IOP is not measured. Currently there is no reliable method of “translating” the output of the strain gauge to the actual IOP. The 24 hour measurements do produce a graph that accurately portrays the intraocular pressure fluctuation over time. This can still be very useful information. For example, using this technology a glaucoma specialist could discover IOP spikes that may occur during times outside of normal office hours. This, in turn, could explain why a patient’s glaucoma is getting worse despite low intraocular pressure measurements in the office.
2) The contact lens may be small, but this miniaturization comes at a price. Small transmitters have weak signals. In order to accurately pick up the data signal the antenna must be very close to the contact lens. SENSIMED has solved this problem by designing an antenna that adheres to the skin around the eye. This antenna is then connected via a wire to the wearable recorder. According to the SENSIMED website, “The patient wears the SENSIMED Triggerfish® system up to 24 hours and assumes normal activities including sleep periods.[2]” However, the illustration provided on the SENSIMED site of a person wearing one of these antennas give one the distinct impression of a cyborg. As such, if I were wearing one of these devices I might choose to limit my “normal activities” to those that can be performed within the walls of my home. I anticipate that most people will share my view and decide to stay home during the 24 hour monitoring period in order to avoid curious stares from strangers.
3) Although it does have the CE mark, it is not approved for use in the USA.Given the glacially slow rate of new medical device approval here in the USA I wouldn’t hold my breath in anticipation of seeing this available to US residents anytime soon.
4) No doubt this technology is expensive to purchase and will, therefore, be expensive to use. As the SENSIMED Trigger?sh® Sensor device is not yet available in the USA I cannot comment on what 24 hour monitoring would cost. Additionally, I wouldn’t expect Medicare or Commercial insurances to cover it right away even if it were approved for use.
Still, considering the above limitations, I am genuinely impressed that this technology is already in use in Europe. If it is ever approved for use in the USA I will be among the first to make it available for my patients with glaucoma.
References:
- Matteo Leonardi, Elie M. Pitchon, Arnaud Bertsch, Philippe Renaud and Andre Mermoud : Wireless contact lens sensor for intraocular pressure monitoring : assessment on enucleated pig eyes. Acta Ophthalmol. 2009 : 87 : 433–437.
- www.sensimed.ch/en/

David Richardson, MD
Medical Director, San Marino Eye
David Richardson, M.D. is recognized as one of the top cataract and glaucoma surgeons in the US and is among an elite group of glaucoma surgeons in the country performing the highly specialized canaloplasty procedure. Morever, Dr. Richardson is one of only a few surgeons in the greater Los Angeles area that performs MicroPulse P3™ "Cyclophotocoagulation" (MP3) glaucoma laser surgery. Dr. Richardson graduated Magna Cum Laude from the University of Southern California and earned his Medical Degree from Harvard Medical School. He completed his ophthalmology residency at the LAC+USC Medical Center/ Doheny Eye Institute. Dr. Richardson is also an Ambassador of Glaucoma Research Foundation.


