MicroPulse® P3 “Cyclophotocoagulation”
There is a new type of minimally invasive glaucoma surgery (MIGS) that has quietly joined the fray in the battle against glaucoma: MicroPulse® P3 “Cyclophotocoagulation” (or “MP3”).
What is MicroPulse® P3 “Cyclophotocoagulation”?
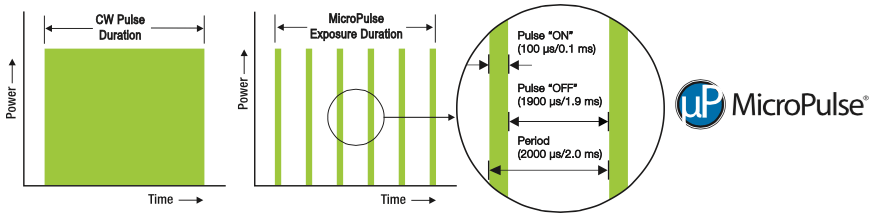
Traditional methods of cyclophotocoagulation burn the ciliary body. MicroPulse® P3 “Cyclophotocoagulation”, however, uses a slow application of laser energy that is “chopped” into micropulses (or, bursts). Each pulse heats up, but does not burn or destroy eye tissue. In between each pulse is a pause. This pause allows the eye tissue to cool off. In this manner the eye tissue is changed rather than destroyed.
Each pulse heats up, but does not burn or destroy eye tissue. In between each pulse is a pause. This pause allows the eye tissue to cool off. In this manner the eye tissue is changed rather than destroyed.
So, if MicroPulse® P3 “Cyclophotocoagulation” is not destroying ciliary body tissue then how does it work? The short answer is that no one really knows. With more traditional forms of cyclophotocoagulation used to treat glaucoma, the ciliary body tissue must be destroyed in order to obtain an intraocular pressure (IOP) lowering effect. [03.30.2017 Update: How Does Micropulse® P3 Cyclophotocoagulation Work?]
How Well Does MicroPulse® “Cyclophotocoagulation” Work?
Short answer: quite well for the majority of those who have this glaucoma laser surgery.
Longer answer: There are now multiple studies that have looked at the IOP reducing effects of MP3. To date, however, there are no longer term (2+ years) results available for general review.
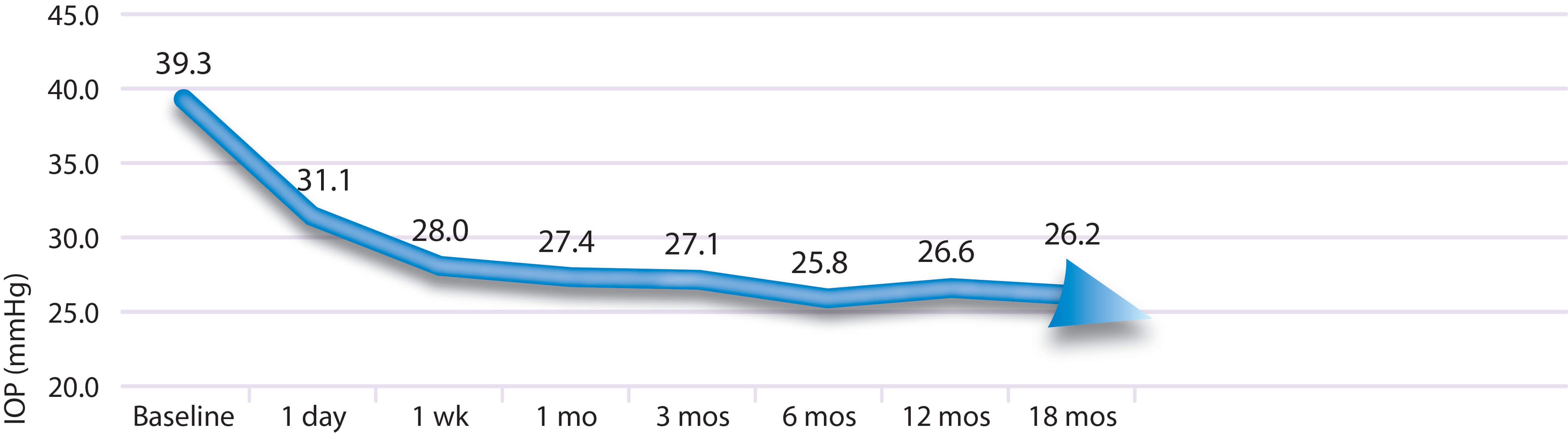
In 2010 results were published documenting the beneficial effect on “refractory glaucoma”. Refractory glaucoma is essentially glaucoma that has not been controlled by any traditional methods of IOP reduction (drops, laser, or surgery including trabeculectomy and “tubes”). This type of glaucoma, as indicated by its name, just does not respond well to treatment. Yet one and a half years out from MicroPulse® P3 “Cyclophotocoagulation” the patients in this study experienced an average drop in IOP of 33% and had (on average) reduced their medication use by almost half (2.1 to 1.3drops).2
NUHS Prospective Clinical Study1
33% IOP reduction at 18 months, (N = 38 patients)
61% med reduction (2.1±1.1 to 1.3±1.0)
More recently, unpublished results of a study performed by Drs. Jessica Maslin and Robert Noecker were presented that further supported the IOP lowering benefit of MicroPulse® P3 “Cyclophotocoagulation” (MP3). In their study of 45 patients with glaucoma, MP3 successfully lowered the IOP by an average of 42% (28.1mmHg —> 16.4mmHg) one year after surgery!
What are the Risks of MicroPulse® P3 “Cyclophotocoagulation”?
Traditional Glaucoma Laser Cyclophotocoagulation has been associated with two main risks: inflammation and hyptotony (an IOP that is too low). Both of these risks can result in loss of vision. This is one of the reasons traditional cyclophotocoagulation is not more commonly recommended. However, because MicroPulse® P3 “Cyclophotocoagulation” (MP3) does not burn or destroy tissue it should not cause significant inflammation.
MicroPulse technology is a tissue-sparing solution where a continuous-wave laser beam is chopped into a train of tiny, repetitive, low energy pulses separated by a brief rest period which allows tissue to cool between laser pulses. | Source: iridex.com
The results of a study comparing MicroPulse® P3 “Cyclophotocoagulation” with continuous (traditional) cyclophotocoagulation were published in 2015.2 Of 24 patients undergoing MP3, none (0%) experienced prolonged hyptony compared to 5 of 24 (21%) who underwent continuous cyclophotocoagulation. Yet both types of laser glaucoma treatment (MP3 and continuous) were effective at lowering IOP by an average of 45% eighteen months after surgery. Additionally, only minimal inflammation was seen with MP3.
There is one other risk that must be mentioned with any newly FDA-approved glaucoma surgery: insurance coverage. Fortunately, as MicroPulse® P3 “Cyclophotocoagulation” is based on a procedure that has been around for decades, it is generally reimbursed by commercial insurances and Medicare without hassle. This makes it unique among minimally-invasive glaucoma surgeries (MIGS).
What is it like to have MicroPulse® P3 “Cyclophotocoagulation”?
MicroPulse® P3 “Cyclophotocoagulation” can be performed in either an office or surgery center. Although there can be some discomfort during the laser application, the procedure is generally not painful. However, unlike other glaucoma laser procedures (such as laser trabeculoplasty), MP3 requires more than just topical anesthetic drops in order to minimize discomfort. Either a local anesthetic “block” (injection around the eye) or intravenous (IV) sedation can be used to achieve adequate comfort during the procedure.
MicroPulse® P3 “Cyclophotocoagulation” is done while in the supine (lying on back) position. Unlike other glaucoma surgeries this procedure can be done even if someone has difficulty lying all the way back due to neck, spine, or breathing difficulty. As such, it is an ideal glaucoma surgery for those with significant medical conditions such as congestive heart failure.
Because there are no incisions (cuts) made in the eye during MicroPulse® P3 “Cyclophotocoagulation” there is no need for sterile draping of the eye. As such, MP3 glaucoma laser surgery is also a good option for anyone who is claustrophobic.
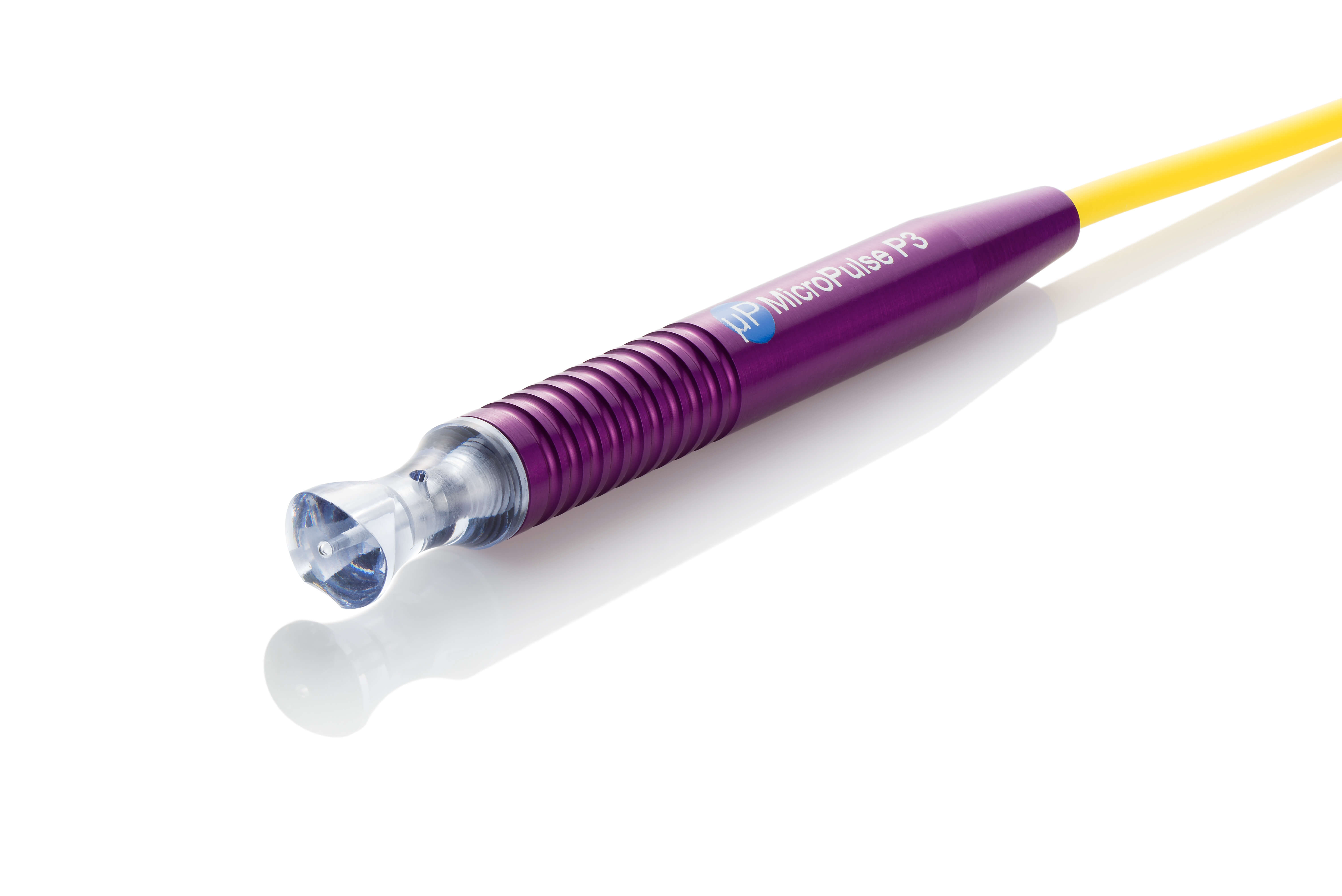
Once adequate anesthesia has been obtained and one is comfortably lying on his or her back, the eyelids are moved out of the way with either a lid speculum or the surgeon’s gloved fingers. The MP3 laser probe is then gently guided along two semi-circular patterns around the front of the eye just beyond where the cornea meets the sclera (white part of the eye). The probe is passed back and forth multiple times. The entire surgery takes only a few minutes.
After surgery the eye may be a little sore. Generally this is mild enough that it can be relieved with acetaminophen or anti-inflammatory eye drops. If IV anesthesia was used then one can expect to be a bit groggy the afternoon of surgery (plan on napping). By the next day, however, most everyone who has chosen MP3 is without significant discomfort or pain.
The eye may also be red after MP3 glaucoma surgery. This is because delicate blood vessels on the surface of the eye may bleed just from the movement of the laser probe along the surface of the eye (especially in those who are taking blood thinners). This “sub-conjunctival hemorrhage” is only of cosmetic concern and will resolve on its own within a week or two of surgery.
Unlike many glaucoma surgeries, there are no restrictions on one’s activities after MicroPulse® P3 “Cyclophotocoagulation”. Nonetheless, it may be prudent to avoid heavy lifting for at least a few days after surgery.
Your surgeon will likely want to see you in his or her office within the first week after surgery. Your IOP may or may not be lower at this first post-operative visit. By one to three months after MP3, however, IOP lowering should be observed. If the IOP is still elevated then a second treatment may be necessary to achieve a reduction in IOP.
What Does MicroPulse® P3 “Cyclophotocoagulation” (MP3) Cost?
For costs or inquiries, please send an email to: [email protected]
Summary
The combination of IOP lowering benefit, low risk profile, and likely reimbursement by commercial insurances and Medicare makes MicroPulse® P3 “Cyclophotocoagulation” a good option for almost all patients with glaucoma who fit into any of the following categories:
- Those with poorly controlled IOP despite using all available glaucoma medications
- Those who have difficulty tolerating glaucoma medications
- Those who have difficulty affording their glaucoma medications
- Those who have difficulty regularly taking their glaucoma medications
- Those who have already had Laser Trabeculolplasty
- Those who are physically unable to tolerate more extensive glaucoma surgery
Given the above list, it’s apparent that almost anyone with glaucoma could benefit from MicroPulse® P3 “Cyclophotocoagulation”.
References:
- Tan AM, Chockalingam M, Aquino MC, Lim ZI, See JL, Chew PT. Micropulse transscleral diode laser cyclophotocoagulation in the treatment of refractory glaucoma. Clin Exp Ophthalmol. 2010 Apr;38(3):266-72. doi: 10.1111/j.1442-9071.2010.02238.x. PubMed PMID: 20447122.
- Aquino MC, Barton K, Tan AM, Sng C, Li X, Loon SC, Chew PT. Micropulse versus continuous wave transscleral diode cyclophotocoagulation in refractory glaucoma: a randomized exploratory study. Clin Exp Ophthalmol. 2015 Jan-Feb;43(1):40-6. doi: 10.1111/ceo.12360. PubMed PMID: 24811050.
Download for Free
 MicroPulse® P3 (MP3) Glaucoma Treatment Patient eBook. Innovative Cyclophotocoagulation with MicroPulse Technology.
MicroPulse® P3 (MP3) Glaucoma Treatment Patient eBook. Innovative Cyclophotocoagulation with MicroPulse Technology.

David Richardson, MD
Medical Director, San Marino Eye
David Richardson, M.D. is recognized as one of the top cataract and glaucoma surgeons in the US and is among an elite group of glaucoma surgeons in the country performing the highly specialized canaloplasty procedure. Morever, Dr. Richardson is one of only a few surgeons in the greater Los Angeles area that performs MicroPulse P3™ "Cyclophotocoagulation" (MP3) glaucoma laser surgery. Dr. Richardson graduated Magna Cum Laude from the University of Southern California and earned his Medical Degree from Harvard Medical School. He completed his ophthalmology residency at the LAC+USC Medical Center/ Doheny Eye Institute. Dr. Richardson is also an Ambassador of Glaucoma Research Foundation.