Introducing Ab-Interno Canaloplasty for Glaucoma
Ab-Interno Canaloplasty: Canaloplasty with an Elegant Twist!
Canaloplasty is a non-penetrating (wall of the eye is not cut all the way through) glaucoma surgery developed by Dr. Robert Stegmann in 2008 with origins dating as far back 1968! It is an advanced surgical treatment for glaucoma which uses the world’s smallest micro-catheter to enlarge the eye’s natural drainage system. It is a safer but similarly effective surgery compared to penetrating surgeries (i.e. Trabeculectomy). More information about Ab-Externo Canaloplasty here
Recently, Dr. Mark Gallardo, developed a less invasive and much faster technique which is possibly as effective as Ab-Externo Canaloplasty: Ab-Interno Canaloplasty (ABiC™). The technique is not as tedious and complicated as the traditional canaloplasty and can be done by any skilled cataract surgeon. By far, in my opinion, ABiC™, is the most promising, of the microinvasive glaucoma surgeries.
VIDEO: Dr. Richardson shares his insights and shows Dr. Gallardo’s ABiC™ surgery
[AB Interno Canaloplasty for Glaucoma. Part 12 of 12 of “What’s New In Glaucoma Surgery” Presentation, a Continuing Education course for Optometrists presented by Patient-Focused Ophthalmologist, Dr. David Richardson on May 20, 2015. ]
Ab-Interno Canaloplasty: Same Technology, Different Technique
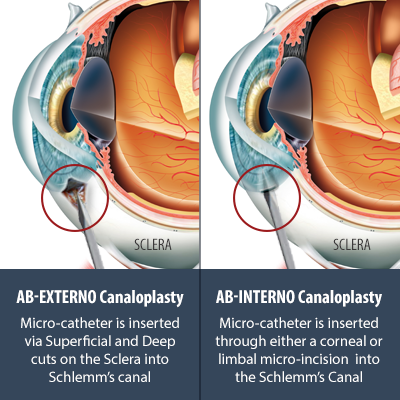
Canaloplasty uses an iTrack™ microcatheter to open the eye’s natural drainage system (“Schlemm’s canal”). Whereas, with traditional Canaloplasty, the Micro-catheter is inserted from an external approach: cutting through the conjuctiva and sclera, with Ab-Interno Canaloplasty, the Micro-catheter is inserted from an internal approach: through either a clear corneal or a limbal micro-incision, then through a small opening in the Trabecular Meshwork, and into the Schlemm’s canal. With Ab-Interno, the eye tissue is preserved and not cut – no more flaps!
The micro-catheter is then routed 360° through the Schlemm’s canal. Once the end of the catheter has circumnavigated to the point of entry, the catheter tip is slowly pulled back while sterile, viscoelastic gel is injected through the catheter and delivered gradually along the canal to dilate it 2-3 times its normal size. This enlarges and breaks down obstructions and adhesion in the canal and restores the natural outflow pathways, without leaving a prolene suture in the Schlemm’s canal (unlike with traditional canaloplasty). Once the outflow pathway is improved, the eye’s fluid can exit through a more natural process allowing the pressure in the eye to drop to a more normal level. (Source: Ellex)
Ab-Interno Canaloplasty: Benefits at a Glance
To date, Ab-Interno Canaloplasty is the only Microinvasive Glaucoma Surgery procedure that successfully addresses all aspects of potential outflow resistance. You get Trabecular Meshwork treated (an opening is created with Ab-Interno), Schlemm’s canal is dilated and Collector channel systems are also re-opened. Hence, you get better aqueous outflow.
- Similar benefits as traditional canaloplasty
- Similar IOP-lowering as tried and true traditional Canaloplasty.
- Restoration of the eye’s natural drainage channels.
- No permanent placement of foreign body – prolene suture, stents or implants, in the eye!
- Future surgery is not compromised
- Easier and quicker 15 minutes Procedure!
- Preserves tissue. No deep cuts or creation of flaps needed!
- Potentially offer better clinical outcomes than any other currently available MIGS procedure.
Ab-Interno Canaloplasty: Is It Safe and Effective?
Ab-Interno Canaloplasty is a microinvasive glaucoma surgery (MIGS) procedure that’s just been developed as an enhancement of Canaloplasty. Canaloplasty has been available for a number years. We have long-term results with the Ab-Externo (traditional) Canaloplasty and they look really good! (See Is Traditional Canaloplasty Safe & Effective?).
The latest ABiC™ technique, developed by Dr. Mark Gallardo in 2015, actually looks really good early on. Below are 12-month case studies of 106 eyes (Dr. Khiami) and 122 eyes (Dr. Gallardo).
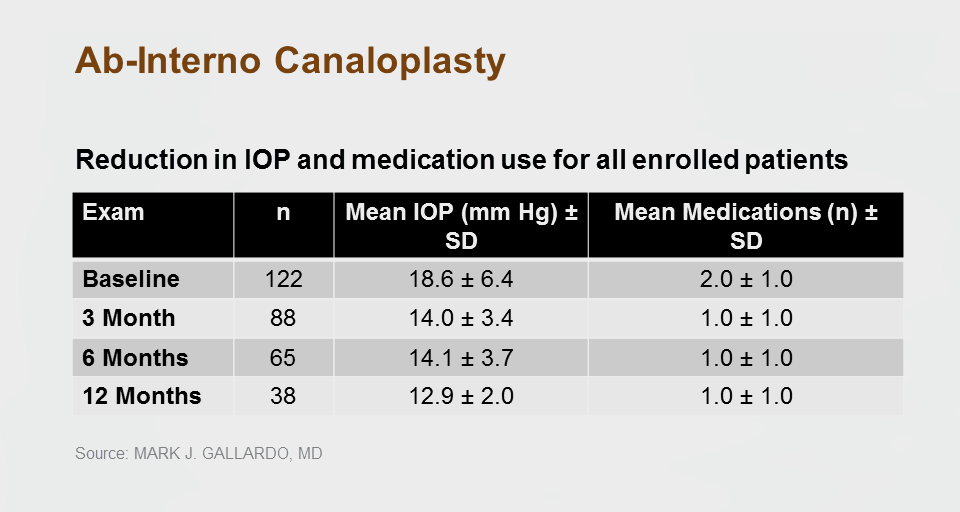
Mark J. Gallardo, MD (El Paso Eye Surgeons, PA) completed a 12-month study to evaluate the effect of ABiC in reducing IOP and dependence on anti-glaucoma medications.
Mean IOP was reduced from 18.6 ± 6.4 mm Hg preoperatively to 12.9 ± 2.0mm Hg (n=28) at 12 months postoperative, a total average reduction in IOP of 30.64%. Additionally, ABiC™ reduced the mean number of medications from 2 ± 1 drops at baseline to 1 ± 1 drops at 12 months postoperative, representing a 50% decrease in medications. (Refer to Table 2.) ABiC™ was found to be effective both combined with cataract surgery and as a standalone procedure. In patients who underwent ABiC™ alone (n=60), mean IOP reduced by 37.55% from 21.3 ±7.4 mm Hg preoperatively to 13.3 ± 2.3 mm Hg at 12 months postoperative (n=6) with a 66.66% reduction in medication use.
Copy Source: http://www.ellex.com/wp-content/uploads/sites/9/ABiC-Whitepaper-12-Months-1.pdf
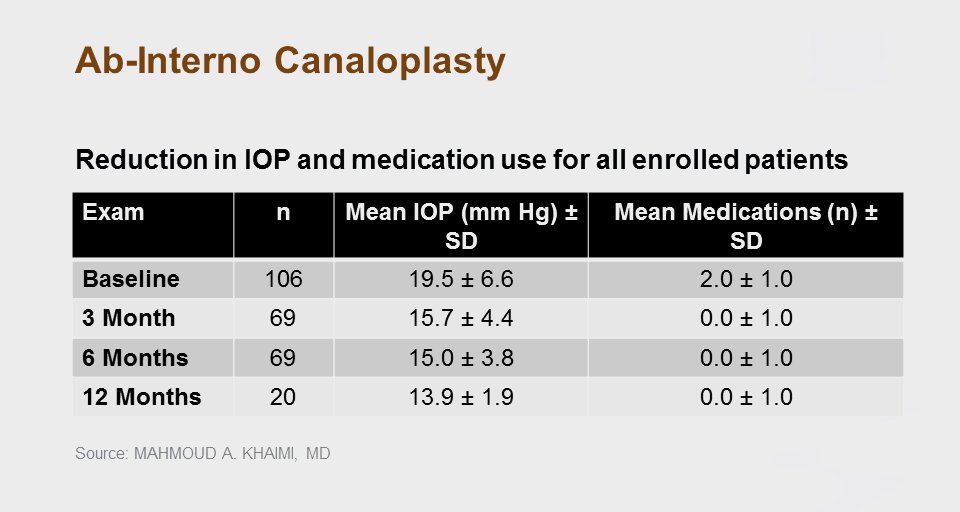
Mahmoud A. Khaimi, MD (Dean McGee Eye Institute, University of Oklahoma), completed a 12-month study to evaluate the effect of ABiC in reducing IOP and dependence on anti-glaucoma medications.
Findings from Dr. Khaimi’s study of 106 patients showed that mean IOP was reduced from 19.5 ± 6.6 mmHg preoperatively, to 15.7 ± 4.4 mm Hg (n=69), 15.0 ± 3.8 mm Hg (n=69) and 13.9 ± 1.9 mm Hg (n=20) at 3, 6 and 12 months postoperative, respectively. Medication dependency reduced from 2 ± 1 drops before ABiC™ to 0 ±1 drops at 3, 6 and 12 months postoperative, representing a total average decrease of 28.7% in IOP and 100% in glaucoma medications.
Copy Source: http://www.ellex.com/wp-content/uploads/sites/9/ABiC-Whitepaper-12-Months-1.pdf
Case observation of ABiC™ also revealed that the safety profile of the procedure was similar to that of traditional Canaloplasty and the newer MIGS procedures. In the 12-month studies by Dr Gallardo and Dr Khaimi, overall, the frequency of surgical and postsurgical complications was low, with no serious adverse events recorded.
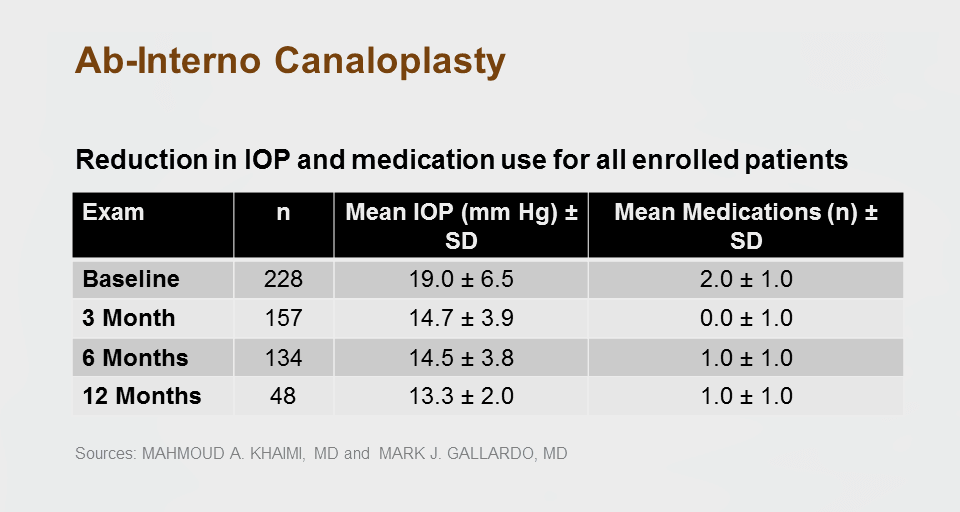
Combining the two cohorts (n= 228 eyes), the mean preoperative IOP was 19.0 ± 6.5 mm Hg and the mean number of medications was 2.0 ± 1.0. At three, six and 12 months post-treatment, mean IOP was 14.7 ± 3.9 mm Hg, 14.5 ± 3.8 mm Hg and 13.3 ± 2.0 mm Hg, respectively, while the mean number of medications was 0.0± 1.0 at three months, and 1.0 ± 1.0 at six and twelve months post-treatment (refer to Table 2). At 12 months (n = 48) the average IOP reduction was 30%, combined with a 50% reduction in the number of medications.
Copy Source: http://www.ellex.com/wp-content/uploads/sites/9/ABiC-Whitepaper-12-Months-1.pdf
Ab-Interno Canaloplasty: Are You a Candidate?
Ab-Interno Canaloplasty is an advanced Microinvasive Glaucoma Surgery (MIGS) procedure, approached “from inside the eye” to lower elevated IOP for patients with mild-to-moderate glaucoma. ABiC™ is also suitable for the following:

- Patients with mild-to-moderate open-angle glaucoma, pigmentary glaucoma, pseudoexfoliation glaucoma, normal tension glaucoma, juvenile glaucoma and steroid induced Glaucoma
- Patients who have undergone selective laser trabeculoplasty (SLT) or single session low power ALT
- Patients with Ocular Hypertension
- Patients who have difficulty using medications
- Patients with previous failed trabeculectomy or tube surgery or in whom glaucoma surgery in the other eye has failed
*** Ab-Interno Canaloplasty is not recommended for patients with neovascular glaucoma, chronic angle closure, angle recession/peripheral anterior synechiae or narrow angle glaucoma, chronic uveitis, and those who have undergone multiple treatments of Argon Laser Trabeculoplasty. ***