Commonly Encountered Risks of Endocyclophotocoagulation (ECP)

ECP treatment with a curved probe via www.ophthalmologymanagement.com
Fortunately, many of the risks associated with Transscleral Cyclophotocoagulation (TCP) are rarely seen after Endocyclophotcoagulation (ECP). However, there are still a few commonly seen and undesired outcomes associated with ECP. Following is an incomplete list of just the more commonly encountered risks.
Intraocular Pressure Elevation (IOP Spike)
As with most glaucoma surgeries, ECP shares the risk of post-operative IOP elevation. Although generally modest and self-limited these post-operative elevations do occasionally require additional medical treatment and (rarely) additional glaucoma surgery to control the IOP.
For example, as I write this post I have a patient who is just over one month out from ECP performed by another surgeon who is, BTW, a very skilled surgeon. Prior to ECP he was taking only one glaucoma medication. He now requires the use of four separate medications to achieve the same IOP control noted prior to ECP using only one medication. I am hopeful that this will resolve with time. However, this experience alone makes me uncomfortable with offering this therapy to my own patients.
Significant Inflammation
Treatment of the ciliary processes actually requires a bit if finesse. Too little treatment and the ciliary process bounces right back with its production of aqueous. Too much treatment and it actually “pops” like a popcorn kernel. The latter can be associated with a severe inflammatory reaction resulting in fibrin strands in the eye. This can happen in about one quarter of those who have ECP. Vision can be temporarily decreased if the fibrin forms a curtain over the pupil. Generally this resolves with topical steroid use.
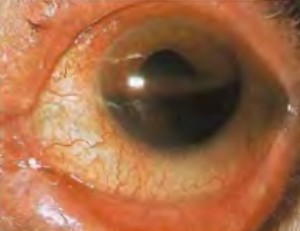
Hyphema By Rakesh Ahuja, MD (Own work) [CC BY-SA 2.5 via Wikimedia Commons
Bleeding in the Eye (Hyphema)
Bleeding in the front part of the eye (called a “hyphema”) can be seen after just about all surgical glaucoma treatments. A hyphema can be expected in approximately 12% of those who have ECP.
Swelling of the Central Retina (Macular Edema)
Inflammation in the eye can result in swelling of the central retina (called “macular edema”) which can then lead to loss of vision if it does not resolve. About one in ten people who have ECP will develop macular edema. Fortunately, this generally resolves with only eye drop treatment.
Loss of Vision
Considering that the entire purpose of glaucoma surgery is to save vision, any risk of loss of vision is serious. Although earlier studies noted vision loss in up to 6% of those who had ECP, such a high risk has not been seen in more recent studies.
Choroidal Detachment
Another risk that is seen in almost all glaucoma surgeries is swelling of the inner lining of the eye (called a “choroidal detachment”). This can be expected in just under 1 in 20 patients who have ECP. Fortunately, choroidal detachments generally resolve with topical (eye drop) treatment. Occasionally, however, surgery is needed to resolve this condition.
References
- Chs BA, Berke SJ, Dustin L, Noecker R. Endoscopic cyclophotocoagulation combined with phacoemulsification versus phacoemulsification alone in medically controlled glaucoma. J Cataract Refract Surg. 2014;40(8):1313-1321.
- Chen J, Cohn RA, Lin SC, et al. Endoscopic photocoagulation of the ciliary body for treatment of refractory glaucomas. Am J Ophthalmol. 1997;124:787-796.
- Francis BA, Berke SJ, Dustin L, Noecker R. Endoscopic cyclophotocoagulation combined with phacoemulsification versus phacoemulsification alone in medically controlled glaucoma. J Cataract Refract Surg. 2014;40(8):1313-1321.

David Richardson, MD
Medical Director, San Marino Eye
David Richardson, M.D. is recognized as one of the top cataract and glaucoma surgeons in the US and is among an elite group of glaucoma surgeons in the country performing the highly specialized canaloplasty procedure. Morever, Dr. Richardson is one of only a few surgeons in the greater Los Angeles area that performs MicroPulse P3™ "Cyclophotocoagulation" (MP3) glaucoma laser surgery. Dr. Richardson graduated Magna Cum Laude from the University of Southern California and earned his Medical Degree from Harvard Medical School. He completed his ophthalmology residency at the LAC+USC Medical Center/ Doheny Eye Institute. Dr. Richardson is also an Ambassador of Glaucoma Research Foundation.


