Well, we now know the effects of canaloplasty will last. At least, we know the effects of canaloplasty will last for three years. And, three years is about as long as any study involving real patients (you know, the type that move, cancel appointments because they are doing fine, or are otherwise lost to follow up) can manage.

Well, we now know the effects of canaloplasty will last. At least, we know the effects of canaloplasty will last for three years. And, three years is about as long as any study involving real patients (you know, the type that move, cancel appointments because they are doing fine, or are otherwise lost to follow up) can manage.
So, just what do the three year results show? Well, the final article has not been published yet, but the results were presented at this year’s annual meeting of glaucoma specialists in Dana Point, California. {{2}} The results were impressive.
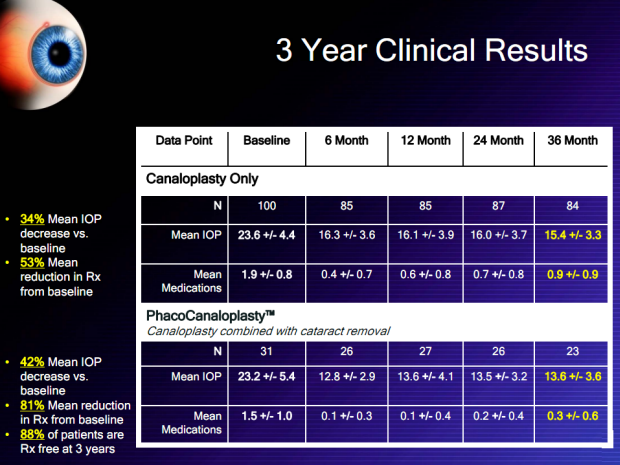
Canaloplasty 3 Year Results – Brief Summary:
1) The reduction in intraocular pressure (IOP) after canaloplasty was 34%. Not only is this a respectable reduction in IOP, but at all time points measured (6, 12, 24, and 36 months), this was the lowest average IOP!
2) The number of medications required to keep the IOP under control was reduced by 53% from baseline. This means that (on average) patients were able to cut the number of glaucoma drops they used in half. Assuming that the average glaucoma patient who needs surgery is spending $200/month on glaucoma medications prior to surgery, this sustained reduction in drops used means that the cost of canaloplasty could easily be paid just with the cost savings from using fewer medications to control IOP.
It gets even better, though, for those patients who have combined canaloplasty plus cataract surgery:
3) The IOP in those patients who underwent Phacocanaloplasty™ was reduced by almost half (42%)! Again, this is three years after surgery!
4) How about the number of drops used? Get ready for this: an 81% reduction (on average) in the number of drops needed to control IOP!
5) There was even a bonus (as if one was needed after reading the above results): an astounding 88% of patients achieved IOP control without drops three years after canaloplasty!
I’m sorry, but any glaucoma surgeon who chooses not to at least give canaloplasty a try after being made aware of these results is either uncertain of his (or her) own skills, or is simply too stuck in his or her ways and should consider an early retirement. With results like these it is simply a disservice to our patients not to present them with an option to trabeculectomy if the IOP goal is in the mid teens and they are candidates for this amazing new surgical treatment for glaucoma.
BTW, I know I will hear it from my colleagues about the above statement but I stand by it. Today, no cataract surgeon would consider not at least informing patients with cataracts of their intraocular lens options. I believe it is now time to give our glaucoma patients some choice in the surgical management of their lifelong disease.


